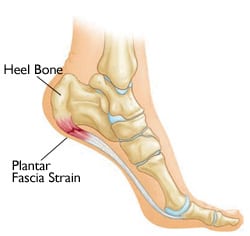
Plantar fasciitis is a common cause of foot pain. The plantar fascia is a ligament that connects your heel bone to your toes. It supports the arch of your foot. When the ligament becomes strained it can become inflamed and cause pain under your heel.
What Does Plantar Fasciitis Feel like?
If you have plantar fasciitis your feet may feel painful and stiff when you wake up in the morning and get out of bed. It usually gets better as you exercise and loosen your foot up but it tends to get worse again at the end of the day.
If you stretch your toes upwards, or stand on tip toe you will notice the pain getting worse. In about 80% of cases people with plantar fasciitis also experience stiffness in their Achilles tendon (the tendon at the back of your ankle). When it first appears it can feel like there is a thickness around the area like something is stuck in your sock. As it progresses it can feel like needles are sticking into your heel when you take a step.
Who is at Risk From Plantar Fasciitis?
- Runners or people who walk long distances.
- People who stand up a lot at work.
- People who are overweight.
- People with tight calf muscles or stiff ankle muscles.
- People who have particularly low or high arches in their feet.
How Can I Prevent It?
When walking or running, keep your strides medium length. A walkers foot should hit the ground in the middle of their heel, not the back. A runner should hit the ground with a midfoot strike. Over reaching your strides and landing with the back of your heel on the floor will create stress on your plantar fascia.
Try and keep to flat surfaces and avoid hills and trails. If you’re serious about running and walking in your free time, or have a job that involves standing all day then take the lift instead of the stairs when you have the option to, it will give your feet a break.
Improve the flexibility of your legs and ankles with stretching exercises and always remember to warm up and cool down. Wearing the right shoes will really help. Your shoes should be soft and flexible. Avoid high heels if you have to walk very far or if you have a job where you need to stand a lot. Needless to say, running in high heels can be very bad for your feet.
How to Ease Acute Pain from Plantar Fasciitis:
- Take a non steroidal anti inflammatory, such as ibuprofen.
- Use an orthotic on your heel, it can help the pain but is not a long term solution.
- Soak your foot in a bowl of cold water and then elevate it, to help reduce swelling.
What Can Be Done About Plantar Fasciitis Long Term?
While plantar fasciitis usually goes away on it’s own with rest, the healing process can take 6 weeks to a year. This can be very frustrating if you are a serious runner or walker, as it means you have to be out of action until you are healed. Even if you take a break from strenuous activity, the average person takes thousands of steps a day and it is unpleasant, to say the least, to have each one of those steps cause you pain. A physiotherapist can help you have a much speedier recovery, as well as helping you identify what exactly has caused the plantar fasciitis so you can be mindful about stopping it from happening in future.
Whilst plantar fasciitis is a common cause of foot pain, it isn’t the only one, so seeing a physiotherapist will help you get the correct diagnosis and rule out any other causes.
To enquire about booking an appointment please call 0114 268 6677 or email info@sheffieldphysiotherapy.co.uk.

